By Aine Cryts
Breast ultrasound is “an evolving technology and field,” says Marc Inciardi, MD, associate professor of radiology and a breast radiology specialist at University of Kansas Medical Center in Kansas City, Kansas. He also calls breast ultrasound “an important adjunct to mammography and to MRI, in some cases.”
He calls on radiologists and radiology leaders to pay attention to the upgrades and advances in technology and research to determine how this emerging technology can help improve patient care. Here are three things Inciardi thinks radiologists should know about breast ultrasound.
Breast ultrasound may provide better cancer screening for certain populations. “By now, most people are aware of the limitations of mammography and, though 3D mammography does improve the screening diagnostic accuracy of all densities, it fails to detect some cancers in patients with dense breast tissue,” Inciardi says. “In certain patient populations, in screenings, breast ultrasound can play a role. Vendors continue to improve their technology, which results in improvements in patient care.”
Patients who are at average or intermediate risk could benefit from use of breast ultrasound, he says. “Generally, high-risk populations are recommended to have MRI. There may be some in that latter population who, for some reason, may not be able to undergo MRI. That could be claustrophobia, having a pacemaker, weight limitations, allergies to gadolinium, and financial issues.”
New technology improves ultrasensitive vascular imaging. While traditional Doppler shows the vascularity of breast lesions, it hasn’t been shown to be useful in differentiating benign breast tissue from cancer, according to Inciardi. Ultrasensitive vascular imaging is a more sensitive technique with higher resolution, he adds.
“Recent research has shown that, in a small series, [ultrasensitive vascular imaging] can play a role in differentiating malignant lesions from benign lesions and help us better characterize lesions and perhaps reduce the number of biopsies Perhaps we might upgrade a lesion that we might have thought wasn’t cancerous to have a biopsy and find the cancer or downgrade a lesion that does not need biopsy,” he says. Inciardoi notes that most vendors offer some form of ultrasensitive vascular imaging technology: “It’s an emerging technology that deserves additional research and a second look by radiologists to see how it works in their practice.”
Automated ultrasound can support radiologists’ efficiency and accuracy. The FDA approved in 2017 a CAD system for automated breast ultrasound. Inciardi is co-author of a research study that shows radiologists could decrease their reading time by about a third with no loss in accuracy of the interpretation.
He has some advice for vendors developing automated ultrasound technologies: “I’d like to see elastography and Doppler added, if it could be done. The idea is that when we see a lesion, it would potentially give us better decision support whether to call the patient back or decide that the lesion is benign and not call them back. Artificial intelligence could use the elastography and doppler—as well as perhaps margin assessment—to include in a decision algorithm to determine if we should call the patient back for a lesion that’s found versus meeting a criteria that says it’s benign and to put the patient back into a regular screening routine for mammography.”
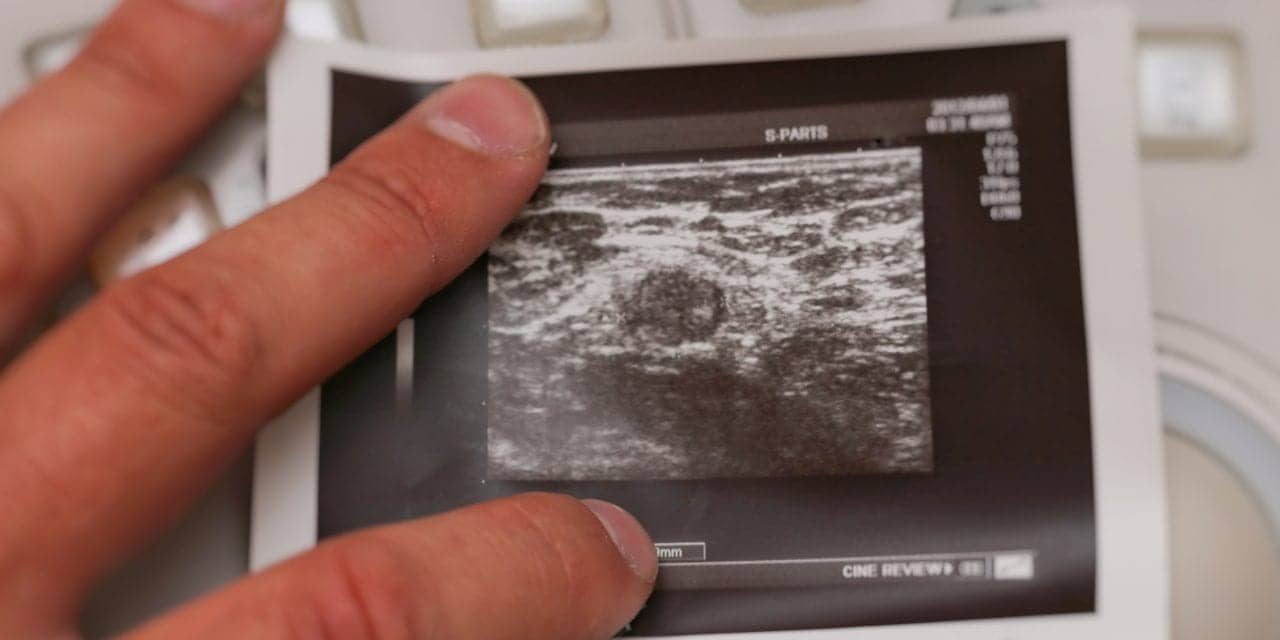
Featured image: Ultrasound photo of metastatic lymph node in breast cancer.