The first study to examine both chest X-ray and CT imaging findings in teenagers with electronic (e-)cigarette or vaping product use-associated lung injury (EVALI) was recently published in the journal Radiology. “This population is particularly vulnerable to e-cigarette use and its potentially life-threatening consequences,” says the study’s lead author, Maddy Artunduaga, MD, assistant professor of pediatric radiology at UT Southwestern Medical Center in Dallas.
First introduced in the U.S. around 2007, e-cigarettes are now the most used tobacco product among U.S. youth. The 2018 National Youth Tobacco Survey reported that in 2018 more than 3.6 million middle and high school students were using e-cigarettes.
Although vaping has been often marketed as a safer alternative to smoking traditional cigarettes, e-cigarette liquids and aerosols contain a variety of chemicals that can result in ill health effects. When these potentially harmful chemicals are inhaled, acute lung injury may occur. EVALI has emerged as a serious and sometimes fatal complication of vaping. Patients under 18 years of age account for 15% of reported U.S. hospitalizations due to EVALI.
Imaging plays a key role in the evaluation of suspected EVALI. Accurate identification of the condition allows for prompt medical treatment, which may decrease the severity of injury in some patients.
Artunduaga and colleagues retrospectively reviewed chest CT images and X-rays of 14 patients (7 boys and 7 girls) ranging in age from 13 to 18 years old. All patients included in this study used an e-cigarette or engaged in dabbing—the practice of inhaling small quantities of a concentrated and vaporized drug, such as cannabis oil—in the 90 days before symptom onset. Four patients had a history of exposure to both tetrahydrocannabinol (THC) and nicotine-containing vaping products. Nine patients had a history of exposure to THC-containing vaping products only. One patient had a history of exposure to nicotine-containing vaping products only.
All 14 patients had respiratory symptoms. Symptoms varied among patients but most commonly included shortness of breath, cough and chest pain. Twelve patients also had gastrointestinal symptoms, such as vomiting, nausea, diarrhea or abdominal pain. Four patients initially had isolated gastrointestinal symptoms and later developed respiratory symptoms after hospital admission. Other symptoms included fever, chills, weight loss and fatigue.
“In some cases, the initial symptoms may lead clinicians to suspect a gastrointestinal origin for the patient’s presentation, and the radiologist may be the first to suggest EVALI as a diagnostic consideration,” Artunduaga says.
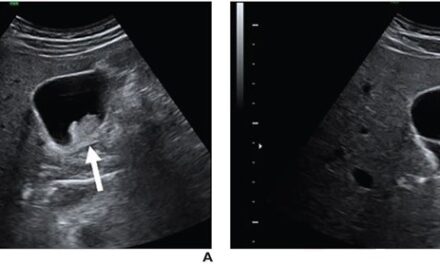
The results showed characteristic chest X-ray and CT findings. Bilateral and symmetric ground-glass opacity in the lungs, frequently associated with consolidation, often of lower lobe predominance, was the key imaging finding. On CT, subpleural sparing was also visualized in 79% of patients.
“Another imaging feature observed on CT in 36% of our pediatric patients with EVALI, was the reversed halo sign, which is characterized by the presence of a central ground-glass opacity surrounded by denser consolidation of crescentic shape or complete ring,” Artunduaga says.
Artunduaga notes that chest X-ray alone does not allow the sufficient characterization of the patterns of EVALI in pediatric patients and, therefore, CT is needed for a complete assessment. “CT provides a better evaluation of the extent and degree of involvement, as well as a better assessment of the characteristics of abnormal pulmonary findings. This can lead to the early diagnosis of EVALI, which would ultimately allow the timely management of this entity in the pediatric population,” she says.
Recent advances in low-dose CT techniques have yielded diagnostic exams that have decreased radiation dose up to 93%. Thus, the radiation dose associated with low-dose CT is justified in the evaluation of suspected EVALI in pediatric patients, according to Artunduaga. “Radiologists will continue to play an important role in the initial detection and follow-up of pediatric patients with EVALI,” she says. “When these imaging findings are observed in pediatric patients, with or without the history of exposure to e-cigarette or vaping products, EVALI should be included as a diagnostic possibility.”